50 mg
For the use of a Registered Medical Practitioner or a Hospital or a Institution only.
CLOMIPRAMINE TABLETS (Clomipramine Hydrochloride) belong to the dibenzazepine class of tricyclic antidepressants, it has antimuscarinic properties and is also potent serotonin reuptake inhibitor. Chemically, Clomipramine Hydrochloride is 3-(3-Chloro-10, 11-dihydro-5H-dibenzo[b,f]azepin-5-yl)-N,N-dimethylpropan-1-amine hydrochloride. The molecular formula is C19H23ClN2, HCl and molecular weight is 351.3.
STRUCTURAL FORMULA :
Its structural formula is :
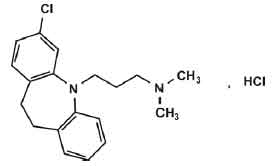
CLOMIPRAMINE TABLETS are white coloured round film coated tablet.
COMPOSITION :
Each film coated tablet contains :
Clomipramine Hydrochloride B.P. 50 mg
Excipients q.s.
Colours : Titanium Dioxide B.P.
ACTIONS :
Clomipramine is a tricyclic antidepressant and its pharmacological action includes alpha-adrenolytic, anticholinergic, anti-histaminic and 5-HT receptor blocking properties. The therapeutic activity of Clomipramine Tablets is thought to be based on its ability to inhibit the neuronal re-uptake of noradrenaline and 5-HT. Inhibition of the latter is the dominant component.
PHARMACOKINETICS :
Absorption :
The active substance is completely absorbed following oral administration and intramuscular injection. The systemic bioavailability of unchanged clomipramine is reduced by 50 % by “first-pass” metabolism to desmethylclomipramine (an active metabolite). The bioavailability of clomipramine is not markedly affected by the ingestion of food but the onset of absorption and therefore the time to peak may be delayed. Coated tablets and sustained release tablets are bioequivalent with respect to amount absorbed. During oral administration of constant daily doses of Clomipramine Tablets the steady state plasma concentrations of clomipramine and desmethylclomipramine (active metabolite) and the ratio between these concentrations show a high variability between patients, e.g. 75 mg Clomipramine Tablets daily produces steady state concentrations of clomipramine ranging from about 20 to 175 mg/ml. Levels of desmethylclomipramine follow a similar pattern but are 40-85 % higher.
Distribution :
Clomipramine is 97.6 % bound to plasma proteins. The apparent volume of distribution is about 12-17 L/kg bodyweight. Concentrations in cerebrospinal fluid are about 2 % of the plasma concentration.
Biotransformation :
The major route of transformation of clomipramine is demethylation to desmethylclomipramine. In addition, clomipramine and desmethylclomipramine are hydroxylated to 8-hydroxy-clomipramine and 8-hydroxy-desmethylclomipramine but little is known about their activity in vivo. The hydroxylation of clomipramine and desmethylclomipramine is under genetic control similar to that of debrisoquine. In poor metabolisers of debrisoquine this may lead to high concentrations of desmethylclomipramine; concentrations of clomipramine are less significantly influenced.
Elimination :
Oral clomipramine is eliminated from the blood with a mean half-life of 21 hours (range 12-36 h), and desmethylclomipramine with a half-life of 36 hours. About two-thirds of a single dose of clomipramine is excreted in the form of water-soluble conjugates in the urine, and approximately one-third in the faeces. The quantity of unchanged clomipramine and desmethylclomipramine excreted in the urine amounts to about 2 % and 0.5 % of the administered dose respectively.
Characteristics in patients :
In elderly patients, plasma clomipramine concentrations may be higher for a given dose than would be expected in younger patients because of reduced metabolic clearance. The effects of hepatic and renal impairment on the pharmacokinetics of clomipramine have not been determined.
INDICATIONS :
More serious depressive conditions which can be treated with clomipramine include major depression (endogenous, unipolar, manic-depressive states, involutional melancholia and masked depression), reactive depression (neurotic depression) and secondary depression (depression associated with alcoholism, schizophrenia, parkinsonism and personality disorders, depression caused by medicines and senility with depression).
Administration :
For oral use.
Dosage :
In the treatment of depression in adults, clomipramine hydrochloride is given in oral doses of 10 mg daily initially,increasing gradually to 30 to 150 mg daily if required; up to 250 mg daily or higher may be given in severe cases. A suggested initial dose for the elderly is 10 mg daily increasing gradually over 10 days to 30 to 75 mg daily if required. Clomipramine may be given in divided doses throughout the day, but since it has a prolonged half-life, once-daily dosage regimens are also suitable, usually given at night. In the treatment of obsessive-compulsive disorder and phobias, clomipramine hydrochloride may be given in an initial oral dose of 25 mg daily (or 10 mg daily for elderly patients or those sensitive to tricyclics) increased gradually over two weeks to 100 to 150 mg daily. In some countries, maximum doses of 250 mg daily have been used. Similar doses have also been used in the management of panic disorder. In some countries clomipramine hydrochloride is also used for the treatment of obsessive-compulsive disorder in children and adolescents aged
10 years and over. In the adjunctive treatment of cataplexy associated with narcolepsy, clomipramine hydrochloride is given in an initial oral dose of 10 mg daily and gradually increased until a satisfactory response occurs, usually within the range of 10 to 75 mg daily.
Clomipramine should be withdrawn gradually to reduce the risk of withdrawal symptoms.
CONTRAINDICATIONS :
Known hypersensitivity to clomipramine, or any of the excipients or cross-sensitivity to tricyclic antidepressants of the dibenzazepine group. Recent myocardial infarction. Any degree of heart block or other cardiac arrhythmias. Mania, severe liver disease, narrow angle glaucoma. Retention of urine. Anafranil should not be given in combination or within 3 weeks before or after treatment with a MAO inhibitor. The concomitant treatment with selective, reversible MAO-A inhibitors, such as moclobamide, is also contra-indicated.
WARNINGS :
This medicine should at all times be kept out of reach of children, as relatively small overdoses may be fatal to them. Caution should be exercised when prescribing tricyclic antidepressants in patients with cardiovascular insufficiency, atrioventricular block (grades I to III) and arrhythmias. narrow-angle glaucoma. disorders of micturition due to an impeded flow of urine (e.g. in diseases of the prostate). a low convulsions threshold (e.g. due to brain damage of varying aetiology, epilepsy, alcoholism). severe hepatic or renal disease. tumours of the adrenal medulla (e.g. phaeochromocytoma, neuroblastoma) in whom the medicine may provoke hypotensive crises Simultaneous treatment of patients with tricyclic antidepressants and electroconvulsive therapy should only be resorted to under careful
supervision.
PRECAUTIONS :
Clomipramine hydrochloride should be administered with caution in patients with urinary retention, prostatic hypertrophy or constipation or in patients with increased intraocular pressure due to its anticholinergic properties. Tricyclic antidepressants are known to lower the convulsive threshold and clomipramine should, therefore, be used with extreme caution in patients with a history of convulsive disorders and other predisposing factors, e.g. brain damage of varying etiology, alcoholism and concomitant use with other medicines that lower the seizure threshold. Clomipramine hydrochloride should be administered with extreme caution to patients with a history of cardiovascular disease. Caution should be observed in prescribing Clomipramine in hyperthyroid patients or in patients receiving thyroid medication cojointly. Depressed patients with suicidal tendencies should be carefully supervised during treatment. Elderly patients and young children can be particularly sensitive to the side-effects and a reduced dose, especially initially, should be employed. Blood sugar concentrations may be altered in diabetics.
Pregnancy : Category C
Neonatal withdrawal symptoms have been reported.
Nursing mothers :
Excreted in breast milk.
Paediatric use:
Not recommended for children < 10 yrs.
EFFECTS ON ABILITY TO DRIVE AND USE MACHINES :
Patients receiving Clomipramine should be warned that blurred vision, drowsiness and other CNS symptoms may occur in which case they should not drive, operate machinery or do anything else which may require alertness or quick actions. Patients should also be warned that consumption of alcohol or other drugs may potentiate these effects.
INTERACTIONS AND INCOMPATIBILITIES :
Interactions :
Anticholinergics : Effects may be increased.
Barbiturates, charcoal : May increase effects of clomipramine.
Cimetidine, fluoxetine, haloperidol, phenothiazine antipsychotics, oral contraceptives : May increase effects of clomipramine.
Clonidine : May result in hypertensive crisis.
CNS depressants : Depressant effects may be additive.
Guanethidine : Antihypertensive effects may be decreased.
MAO inhibitors : Sweating, convulsions and death may occur.
Incompatibilities : Not applicable.
SIDE EFFECTS :
The most commonly observed adverse events were gastrointestinal complaints, including dry mouth, constipation, nausea, dyspepsia and anorexia; nervous system complaints, including somnolence, tremor, dizziness, nervousness and myoclonus; genitourinary complaints, including changed libido, ejaculatory failure, impotence and micturition disorder and other miscellaneous complaints, including fatigue, sweating, increased appetite, weight gain and Visual Changes. Neurological - ataxia, headache, delirium, speech disorders, muscle weakness, muscle hypertonia, tinnitus, paraesthesia of the extremities, convulsions, EEG changes, hyperpyrexia, Peripheral neuropathy has been reported with other tricyclic antidepressants. Behavioural - drowsiness, fatigue, restlessness, confusion accompanied by disorientation, anxiety states, agitation, sleep disturbances, insomnia, nightmares, aggravated depression, hypomania or manic episodes, disturbed concentration, visual hallucinations, impaired memory, aggressiveness, yawning, personalisation, activation of latent psychosis, delusions. Cardiovascular - orthostatic hypotension with associated vertigo, sinus tachycardia, palpitations. ECG changes in patients with normal cardiac status, arrhythmias, hypertension, conduction disorders, syncope.
Haematologic - leucopenia, agranulocytosis, thrombocytopenia, eosinophilia and purpura. Gastrointestinal - vomiting abdominal pain, diarrhoea, taste perversion, elevated transaminases, stomatitis, obstructive jaundice, hepatitis with or without jaundice.
Endocrine - weight loss, breast enlargement and galactorrhoea in the female, inappropriate antidiuretic hormone (ADH) secretion syndrome, gynecomastia in the male, changes in blood sugarlevels,increase in prolactin levels, menstrual irregularity.
Allergic or toxic - allergic skin reactions (skin rash, urticaria), photosensitisation, pruritus, oedema,drug fever.
Withdrawal symptoms - abrupt cessation of treatment after prolonged administration may occasionally produce nausea, vomiting, abdominal pain, diarrhoea, insomnia, nervousness, anxiety, headache and malaise.
OVERDOSAGE :
The signs and symptoms of overdose with Clomipramine Tablets are similar to those reported with other tricyclic antidepressants. Cardiac abnormalities and neurological disturbances are the main complications. In children accidental ingestion of any amount should be regarded as serious and potentially fatal.
Signs and symptoms : Symptoms generally appear within 4 hours of ingestion and reach maximum severity after 24 hours. Owing to delayed absorption (anticholinergic effect), long half-life, and enterohepatic recycling of the drug, the patient may be at risk for up to 4-6 days. The following signs and symptoms may be seen :
Central nervous system : Drowsiness, stupor, coma, ataxia, restlessness, agitation, enhanced reflexes, muscular rigidity, choreoathetoid movements, convulsions, Serotonin Syndrome (e.g. hypertensive crisis, hyperpyrexia, myoclonus, delirium and coma) may be observed.
Cardiovascular system : Hypotension, tachycardia, QTc prolongation and arrhythmia including Torsade de Pointes, conduction disorders, shock, heart failure; in very rare cases cardiac arrest. Respiratory depression, cyanosis, vomiting, fever, mydriasis, sweating and oliguria or anuria may also occur.
TREATMENT OF OVERDOSAGE :
There is no specific antidote, and treatment is essentially symptomatic and supportive. Anyone suspected of receiving an overdose of Clomipramine Tablets, particularly children, should be hospitalised and kept under close surveillance for at least 72 hours. Perform gastric lavage or induce vomiting as soon as possible if the patient is alert. If the patient has impaired consciousness, secure the airway with a cuffed endotracheal tube before beginning lavage, and do not induce vomiting. These measures are recommended for up to 12 hours or even longer after the overdose, since the anticholinergic effect of the drug may delay gastric emptying. Administration of activated charcoal may help to reduce drug absorption. Treatment of symptoms is based on modern methods of intensive care, with continuous monitoring of cardiac function, blood gases, and electrolytes and, if necessary, emergency measures such as : anticonvulsive therapy, artificial respiration, insertion of a temporary cardiac pacemaker, plasma expander, dopamine or dobutamine ministered by intravenous drip, resuscitation.
Treatment of Torsade de Pointes.
If Torsade de Pointes should occur during treatment with Clomipramine Tablets, the drug should be discontinued and hypoxia, electrolyte abnormalities and acid base disturbances should be corrected. Persistent Torsade de Pointes may be treated with magnesium sulphate 2 g (20 ml of 10 % solution) intravenously over 30-120 seconds, repeated twice at intervals of 5-15 minutes if necessary. Alternatively, if these measures fail, the arrhythmia may be abolished by increasing the underlying heart rate. This can be achieved by atrial and ventricular pacing or by isoprenaline (isproterenol) infusion to achieve a heart rate of 90-110 beats/minute. Torsade de Pointes is usually not helped by antiarrhythmic drugs and those which prolong the QTc interval (e.g. amiodarone, quinidine) may make it worse.
Since it has been reported that physostigmine may cause severe bradycardia, asystole and seizures, its use is not recommended in cases of overdosage with Clomipramine Tablets. Haemodialysis or peritoneal dialysis are ineffective because of the low plasma concentrations of clomipramine.
STORAGE :
Store below 30°C (86°F). protected from moisture and light.
Do not refrigerate.
SHELF LIFE :
24 months from the date of manufacture.
PRESENTATION :
CLOMIPRAMINE TABLETS is available as film coated tablets containing Clomipramine Hydrochloride B.P. 50 mg.
100 tablets in HDPE Bottle with child resistant cap.
Disclaimer : For the use of a Registered Medical Practitioner or a Hospital or a Institution only. Also it is not intended to be used by healthcare professionals or patients for the purpose of prescribing or administering these products. Questions regarding the complete and current content of product labeling / specification / presentation should be directed to SGPharma.

 Cardiovascular
Cardiovascular