0.2 mg/ml
For the use of a Registered Medical Practitioner or a Hospital or a Institution only.
GLYCOPYRROLATE INJECTION USP (Glycopyrrolate) is a anticholinergic (antimuscarinic) agent. Chemically, Glycopyrrolate is Pyrrolidinium, 3-[(SR)-(cyclopentylhydroxyphenylacetyl)oxy]-1,1-dimethyl-, [RS-] bromide. The molecular formula is C19H28BrNO3 and molecular weight is 398.33.
STRUCTURAL FORMULA :
Its structural formula is :
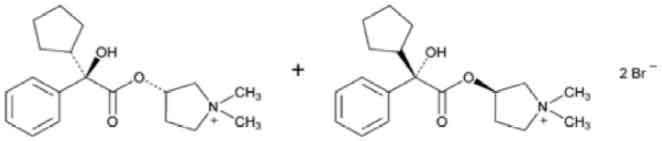
GLYCOPYRROLATE INJECTION USP is a sterile, clear, colourless solution filled in amber ampoule of suitable size.
COMPOSITION :
Each ml contains :
Glycopyrrolate USP 200 mcg
Sodium Chloride USP 7.47 mg
Benzyl Alcohol USP 0.9 % v/v
(as preservative)
Water for Injection USP q.s.
ACTIONS :
Glycopyrrolate is a quaternary ammonium antimuscarinic agent and like other anticholinergic agents, it inhibits the action of acetylcholine on structures innervated by postganglionic cholinergic nerves and on smooth muscles that respond to acetylcholine but lack cholinergic innervation. These peripheral cholinergic receptors are present in the autonomic effector cells of smooth muscle, cardiac muscle, the sinoatrial node, the atrioventricular node, exocrine glands and to a limited degree in the autonomic ganglia. Thus it diminishes the volume and free acidity of gastric secretions and controls excessive pharyngeal, tracheal and bronchial secretions. Glycopyrrolate antagonizes muscarinic symptoms (e.g. bronchorrhea, bronchospasm, bradycardia and intestinal hypermotility) induced by cholinergic drugs such as the anticholinesterases.
The highly polar quaternary ammonium group of glycopyrrolate limits its passage across lipid membranes, such as the blood-brain barrier, in contrast to atropine sulphate and scopolamine hydrobromide, which are non-polar tertiary amines which penetrate lipid barriers easily. Glycopyrronium Injection has been used successfully as an adjunct to reversal by neostigmine when atropine has been used as the preoperative anticholinergic. The use of Glycopyrronium Injection as an adjunct to reversal by neostigmine of non-depolarising muscle relaxants is associated with less initial tachycardia and better protection against the cholinergic effects of neostigmine compared to reversal with a mixture of neostigmine and atropine.
PHARMACOKINETICS :
The following pharmacokinetic information and conclusions were obtained from published studies that used nonspecific assay methods.
Distribution :
The mean volume of distribution of glycopyrrolate was estimated to be 0.42 ± 0.22 L/kg.
Metabolism :
The in vivo metabolism of glycopyrrolate in humans has not been studied.
Excretion :
The mean clearance and mean T1/2 values were reported to be 0.54 ± 0.14 L/kg/hr and 0.83 ± 0.13 hr, respectively post IV administration. After IV administration of a 0.2 mg radiolabeled glycopyrrolate, 85 % of dose recovered was recovered in urine 48 hours postdose and some of the radioactivity was also recovered in bile. After IM administration of glycopyrrolate to adults, the mean T1/2 value is reported to be between 0.55 to 1.25 hrs. Over 80 % of IM dose administered was recovered in urine and the bile as unchanged drug and half the IM dose is excreted within 3 hrs. The following table summarizes the mean and standard deviation of pharmacokinetic parameters from a study.
SPECIAL POPULATIONS :
Gender :
Gender differences in pharmacokinetics of glycopyrrolate have not been investigated.
Renal Impairment : In one study glycopyrrolate was administered IV in uraemic patients undergoing renal transplantation. The mean elimination half-life was significantly longer (46.8 minutes) than in healthy patients (18.6 minutes). The mean area-under-the-concentration-time curve (10.6 hr-µg/L), mean plasma clearance (0.43 L/hr/kg), and mean 3-hour urine excretion (0.7 %) for glycopyrrolate were also significantly different than those of controls (3.73 hr-µg/L, 1.14 L/hr/kg, and 50 %, respectively). These results suggest that the elimination of glycopyrrolate is severely impaired in patients with renal failure.
Hepatic Impairment : Pharmacokinetic information in patients with hepatic impairment is unavailable.
Paediatrics : Following IV administration (5 µg/kg glycopyrrolate) to infants and children, the mean T1/2 values were reported to be between 21.6 and 130.0 minutes and between 19.2 and 99.2 minutes, respectively.
INDICATIONS :
In Anaesthesia :
GLYCOPYRROLATE INJECTION USP is indicated for use as a preoperative antimuscarinic to reduce salivary, tracheobronchial, and pharyngeal secretions; to reduce the volume and free acidity of gastric secretions; and to block cardiac vagal inhibitory reflexes during induction of anaesthesia and intubation. When indicated, GLYCOPYRROLATE INJECTION USP may be used intraoperatively to counteract surgically or drug-induced or vagal reflexes associated arrhythmias. Glycopyrrolate protects against the peripheral muscarinic effects (e.g., bradycardia and excessive secretions) of cholinergic agents such as neostigmine and pyridostigmine given to reverse the neuromuscular blockade due to non-depolarizing muscle relaxants.
In Peptic Ulcer :
For use in adults as adjunctive therapy for the treatment of peptic ulcer when rapid anticholinergic effect is desired or when oral medication is not tolerated.
Administration :
GLYCOPYRROLATE INJECTION USP may be administered intramuscularly, or intravenously, without dilution.
INSTRUCTIONS FOR USE OF AMPOULE :
The ampoule used in this product is equipped with O.P.C. (One Point Cut) opening system. No ampoule file is needed to open the ampoule. The neck of the ampoule is prescored at the point of constriction. A coloured dot on the ampoule head helps to orientate the ampoule. Take the ampoule and face the coloured dot. Let the solution at the head of the ampoule to flow down by shaking or a gentle stroke. The ampoule opens easily by placing the thumb on the coloured dot and gently pressing downwards as shown.

Dosage :
Adults :
Preanaesthetic Medication : The recommended dose of GLYCOPYRROLATE INJECTION USP is 0.004 mg/kg by intramuscular injection, given 30 to 60 minutes prior to the anticipated time of induction of anaesthesia or at the time the preanaesthetic narcotic and/or sedative are administered.
Intraoperative Medication :
GLYCOPYRROLATE INJECTION USP may be used during surgery to counteract drug-induced or vagal reflexes and their associated arrhythmias (e.g., bradycardia). It should be administered intravenously as single doses of 0.1 mg and repeated, as needed, at intervals of 2 to 3 minutes. The usual attempts should be made to determine the etiology of the arrhythmia, and the surgical or anaesthetic manipulations necessary to correct parasympathetic imbalance should be performed.
Reversal of Neuromuscular Blockade :
The recommended dose of GLYCOPYRROLATE INJECTION USP is 0.2 mg for each 1.0 mg of neostigmine or 5.0 mg of pyridostigmine. In order to minimize the appearance of cardiac side effects, the drugs may be administered simultaneously by intravenous injection and may be mixed in the same syringe.
Peptic Ulcer :
The usual recommended dose of GLYCOPYRROLATE INJECTION USP is 0.1 mg administered at 4-hour intervals, 3 or 4 times daily intravenously or intramuscularly. Where more profound effect is required, 0.2 mg may be given. Some patients may need only a single dose, and frequency of administration should be dictated by patient response up to a maximum of four times daily.
lntraoperative Medication :
Because of the long duration of action of GLYCOPYRROLATE INJECTION USP if used as preanaesthetic medication, additional GLYCOPYRROLATE INJECTION USP for anticholinergic effect intraoperatively is rarely needed; in the event it is required the recommended paediatric dose is 0.004 mg/kg intravenously, not to exceed 0.1 mg in a single dose which may be repeated, as needed, at intervals of 2 to 3 minutes. The usual attempts should be made to determine the etiology of the arrhythmia, and the surgical or anaesthetic manipulations necessary to correct parasympathetic imbalance should be performed.
Reversal of Neuromuscular Blockade :
The recommended paediatric dose of GLYCOPYRROLATE INJECTION USP is 0.2 mg for each 1.0 mg of neostigmine or 5.0 mg of pyridostigmine. In order to minimize the appearance of cardiac side effects, the drugs may be administered simultaneously by intravenous injection and may be mixed in the same syringe.
Peptic Ulcer :
GLYCOPYRROLATE INJECTION USP is not recommended for the treatment of peptic ulcer in paediatric patients.
DILUENT COMPATIBILITIES :
Dextrose 5 % and 10 % in water, or saline, dextrose 5 % in sodium chloride 0.45 %, sodium chloride 0.9 %, and Ringer’s Injection.
DILUENT INCOMPATIBILITIES :
Lactated Ringer’s solution.
ADMIXTURE COMPATIBILITIES :
Physical Compatibility : This list does not constitute an endorsement of the clinical utility or safety of coadministration of glycopyrrolate with these drugs. GLYCOPYRROLATE INJECTION USP is compatible for mixing and injection with the following injectable dosage forms : atropine sulfate, physostigmine salicylate, diphenhydramine HCl, codeine phosphate, benzquinamide HCl, hydromorphone HCl, droperidol, levorphanol tartrate, lidocaine, meperidine HCl, pyridostigmine bromide, morphine sulfate, nalbuphine HCl, oxymorphone HCl, procaine HCl, promethazine HCl, neostigmine methylsulfate, scopolamine HBr, butorphanol tartrate, fentanyl citrate, trimethobenzamide HCl, and hydroxyzine HCl. GLYCOPYRROLATE INJECTION USP may be administered via the tubing of a running infusion of normal saline.
ADMIXTURE INCOMPATIBILITIES :
Physical Incompatibility : Since the stability of glycopyrrolate is questionable above a pH of 6.0 do not combine GLYCOPYRROLATE INJECTION USP in the same syringe with methohexital sodium; chloramphenicol sodium succinate; dimenhydrinate; pentobarbital sodium; thiopental sodium; secobarbital sodium; diazepam; dexamethasone sodium phosphate; or pentazocine lactate. These mixtures will result in a pH higher than 6.0 and may result in gas production or precipitation.
CONTRAINDICATIONS :
Known hypersensitivity to glycopyrrolate or any of its inactive ingredients. In addition, in the management of peptic ulcer patients, because of the longer duration of therapy, GLYCOPYRROLATE INJECTION USP may be contraindicated in patients with the following concurrent conditions : glaucoma; obstructive GLYCOPYRROLATE INJECTION USP is not recommended for the treatment of peptic ulcers in paediatric patients.
Paediatric Patients :
Preanaesthetic Medication : The recommended dose of GLYCOPYRROLATE INJECTION USP in paediatric patients is 0.004 mg/kg intramuscularly, given 30 to 60 minutes prior to the anticipated time of induction of anaesthesia or at the time the preanaesthetic narcotic and/or sedative are administered uropathy (for example, bladder neck obstruction due to prostatic hypertrophy); obstructive disease of the gastrointestinal tract (as in achalasia, pyloroduodenal stenosis, etc.); paralytic ileus, intestinal atony of the elderly or debilitated patient; unstable cardiovascular status in acute haemorrhage; severe ulcerative colitis; toxic megacolon complicating ulcerative colitis; myasthenia gravis.
WARNINGS AND PRECAUTIONS :
This drug should be used with great caution, if at all, in patients with glaucoma.GLYCOPYRROLATE INJECTION USP may produce drowsiness or blurred vision. The patient should be cautioned regarding activities requiring mental alertness such as operating a motor vehicle or other machinery or performing hazardous work while taking this drug. In addition, in the presence of fever, high environmental temperature and/or during physical exercise, heat prostration can occur with use of anticholinergic agents including glycopyrrolate (due to decreased sweating), particularly in children and the elderly. Diarrhoea may be an early symptom of incomplete intestinal obstruction, especially in patients with ileostomy or colostomy. In this instance treatment with GLYCOPYRROLATE INJECTION USP would be inappropriate and possibly harmful. GLYCOPYRROLATE INJECTION USP contains benzyl alcohol as preservative. Benzyl alcohol has been reported to be associated with a fatal “Gasping Syndrome” in premature infants. Symptoms include a striking onset of gasping syndrome, hypotension, bradycardia and cardiovascular collapse.
PRECAUTIONS :
General :
Investigate any tachycardia before giving Glycopyrrolate Injection since an increase in the heart rate may occur. Use with caution in patients with: coronary artery disease; congestive heart failure; cardiac arrhythmias; hypertension; hyperthyroidism. Use with caution in patients with renal disease since the renal elimination of glycopyrrolate may be severely impaired in patients with renal failure. Dosage adjustments may be necessary. Use glycopyrrolate with caution in the elderly and in all patients with autonomic neuropathy, hepatic disease, ulcerative colitis, prostic hypertrophy, or hiatal hernia, since anticholinergic drugs may aggravate these conditions. The use of anticholinergetic drugs in the treatment of gastric ulcer may produce a delay in gastric emptying due to antral statis.
Pregnancy : Category B
Reproduction studies with glycopyrrolate were performed in rats at a dietary dose of approximately 65 mg/kg/day (exposure was approximately 320 times the maximum recommended daily human dose of 2 mg on a mg/m2 basis) and rabbits at intramuscular doses of up to 0.5 mg/kg/day (exposure was approximately 5 times the maximum recommended daily human dose on a mg/m2 basis). These studies produced no teratogenic effects to the foetus. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed. Single-dose studies in humans found that very small amounts of glycopyrrolate passed the placental barrier.
Nonteratogenic Effects :
Published literature suggest the following regarding the use of glycopyrrolate during pregnancy. Unlike atropine, glycopyrrolate in normal doses (0.004 mg/kg) does not appear to affect foetal heart rate or foetal heart rate variability to a significant degree. Concentrations of glycopyrrolate in umbilical venous and aterial blood and in the amniotic fluid are low after intramuscular administration to parturients. Therefore, glycopyrrolate does not appear to penetrate through the placental barrier in significant amounts. In reproduction studies in rats, dietary administration of glycopyrrolate resulted in diminished rats of pup survival in a dose-related manner.
Nursing Mothers :
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when GLYCOPYRROLATE INJECTION USP is administered to a nursing woman. As with other anticholinergics, glycopyrrolate may cause suppression of lactation.
Paediatric Use :
Due to its benzyl alcohol content, GLYCOPYRROLATE INJECTION USP should not be used in neonates, i.e., patients less than 1 month of age. Safety and effectiveness in paediatric patients below the age of 16 years have not been established. Safety and effectiveness in paediatric patients have not been established for the management of peptic ulcer. Dysrhythmias associated with the use of glycopyrrolate intravenously as a premedicant or during anaesthesia have been observed in paediatric patients. Infants, patients with Down’s syndrome, and paediatric patients with spastic paralysis or brain damage may experience an increased response to anticholinergics, thus increasing the potential for side effects.
A paradoxical reaction characterized by hyperexcitability may occur in paediatric patients taking large doses of anticholinergics including GLYCOPYRROLATE INJECTION USP. Infants and young children are especially susceptible to the toxic effects of anticholinergics.
Benzyl alcohol, a component of this drug product, has been associated with serious adverse events and death, particularly in paediatric patients. The “gasping syndrome,” (characterized by central nervous system depression, metabolic acidosis, gasping respirations, and high levels of benzyl alcohol and its metabolites found in the blood and urine) has been associated with benzyl alcohol dosages > 99 mg/kg/day in neonates and low-birth-weight neonates. Additional symptoms may include gradual neurological deterioration, seizures, intracranial haemorrhage, haematologic abnormalities, skin breakdown, hepatic and renal failure, hypotension, bradycardia, and cardiovascular collapse.
Although normal therapeutic doses of this product deliver amounts of benzyl alcohol that are substantially lower than those reported in association with the “gasping syndrome,” the minimum amount of benzyl alcohol at which toxicity may occur is not known. Premature and low-birthweight infants, as well as patients receiving high dosages, may be more likely to develop toxicity. Practitioners administering this and other medications containing benzyl alcohol should consider the combined daily metabolic load of benzyl alcohol from all sources.
INTERACTIONS AND INCOMPATIBILITIES :
The effects of atropine and other antimuscarinics may be enhanced by use with other drugs having antimuscarinic properties, such as amantadine, some antihistamines, phenothiazine antipsychotics, and tricyclic antidepressants.Inhibition of drug-metabolising enzymes by MAOIs may possibly enhance the effects of antimuscarinics.The reduction in gastric motility caused by antimuscarinics may affect the absorption of other drugs. Antimuscarinics may also antagonise the gastrointestinal effects of cisapride, domperidone, and metoclopramide. Antimuscarinics and parasympathomimetics may counteract each others effects. Concomitant administration of GLYCOPYRROLATE INJECTION USP and potassium chloride in a wax matrix may increase the severity of potassium chloride-induced gastrointestinal lesions as a result of a slower gastrointestinal transit time.
SIDE EFFECTS :
Anticholinergics, including GLYCOPYRROLATE INJECTION USP, can produce certain effects, most of which are extensions of their pharmacologic actions. Adverse reactions may include xerostomia (dry mouth); urinary hesitancy and retention; blurred vision and photophobia due to mydriasis (dilation of the pupil); cycloplegia; increased ocular tension; tachycardia; palpitation; decreased sweating; loss of taste; headache; nervousness; drowsiness; weakness; dizziness; insomnia; nausea; vomiting; impotence; suppression of
lactation; constipation; bloated feeling; severe allergic reactions including anaphylactic/anaphylactoid reactions; hypersensitivity; urticaria, pruritus, dry skin and other dermal manifestations; some degree of mental confusion and/or excitement, especially in elderly persons. In addition, the following adverse events have been reported from post-marketing experience with glycopyrrolate : malignant hyperthermia; cardiac arrhythmias (including bradycardia, ventricular tachycardia, ventricular fibrillation); cardiac arrest; hypertension; hypotension; seizures; and respiratory arrest. Postmarketing reports have included cases of heart block and QTc interval prolongation associated with the combined use of glycopyrrolate and an anticholinesterase. Injection site reactions including pruritus, oedema, erythema, and pain have also been reported.Glycopyrrolate is chemically a quaternary ammonium compound; hence, its passage across lipid membranes, such as the blood-brain barrier is limited in contrast to atropine sulfate and scopolamine hydrobromide. For this reason the occurrence of CNS-related side effects is lower, in comparison to their incidence following administration of anticholinergics which are chemically tertiary amines that can cross this barrier readily.
INFORMATION FOR PATIENTS :
Because GLYCOPYRROLATE INJECTION USP may produce drowsiness or blurred vision, the patient should be cautioned not to engage in activities requiring mental alertness and/or visual acuity such as operating a motor vehicle or other machinery, or performing hazardous work while taking this drug. The patient also should be cautioned about the use of this drug during exercise or hot weather since overheating may result in heat stroke. The patient may experience a possible sensitivity of the eyes to light.
OVERDOSAGE :
Since glycopyrrolate is a quaternary ammonium agent, symptoms of overdosage are peripheral rather than central in nature.
The other symptoms of overdosage include :
1) CNS symptoms : Excitement, restlessness, convulsions, psychotic behaviour.
2) Hypotension.
3) Curare-like action i.e. neuromuscular blockade leading to muscular weakness and possible paralysis.
TREATMENT OF OVERDOSAGE :
To combat peripheral anticholinergic effects, a quaternary ammonium anticholinesterase such as neostigmine methylsulfate (which does not cross the blood-brain barrier) may be given intravenously in increments of 0.25 mg in adults. This dosage may be repeated every five to ten minutes until anticholinergic overactivity is reversed or up to a maximum of 2.5 mg. Proportionately smaller doses should be used in paediatric patients. Indication for repetitive doses of neostigmine should be based on close monitoring of the decrease in heart rate and the return of bowel sounds. If CNS symptoms (e.g., excitement, restlessness, convulsions, psychotic behaviour) occur, physostigmine (which does cross the blood–brain barrier) may be used. Physostigmine 0.5 to 2 mg should be slowly administered intravenously and repeated as necessary up to a total of 5 mg in adults. Proportionately smaller doses should be used in paediatric patients.
To combat hypotension, administer IV fluids and/or pressor agents along with supportive care. Fever should be treated symptomatically Following overdosage, a curare-like action may occur, i.e., neuromuscular blockade leading to muscular weakness and possible paralysis. In the event of a curare-like effect on respiratory muscles, artificial respiration should be instituted and maintained until effective respiratory action returns.
PHARMACEUTICAL PRECAUTIONS :
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. If visibly opaque particles, discoloration or other foreign particulates are observed, the solution should not be used.
STORAGE :
Store below 30°C (86°F), protected from light.
Do not refrigerate.
SHELF LIFE :
24 months from the date of manufacture.
PRESENTATION :
GLYCOPYRROLATE INJECTION USP is supplied as 200 mcg of Glycopyrrolate USP in 1 ml aqueous solution.
Single Ampoule per Box.
Disclaimer : For the use of a Registered Medical Practitioner or a Hospital or a Institution only. Also it is not intended to be used by healthcare professionals or patients for the purpose of prescribing or administering these products. Questions regarding the complete and current content of product labeling / specification / presentation should be directed to SGPharma.

 Cardiovascular
Cardiovascular