
100 mg
For the use of a Registered Medical Practitioner or a Hospital or a Institution only.
PHENYTOIN TABLETS B.P. (Phenytoin Sodium) is a hydantoin derivative anticonvulsant. The chemical name is Sodium 4-oxo-5,5-diphenyl-4,5-dihydro-1H-imidazol-2-olate. The molecular formula is C15H11N2NaO2 and molecular weight is 274.3.
STRUCTURAL FORMULA :
Its structural formula is :
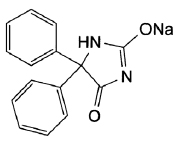
PHENYTOIN TABLETS B.P. are white coloured, circular film coated tablets.
COMPOSITION :
Each film coated tablet contains :
Phenytoin Sodium B.P. 100 mg
Excipients q.s.
Colour : Titanium Dioxide B.P.
ACTIONS :
Phenytoin Sodium inhibits the spread of seizure activity in the motor cortex. It appears that by promoting sodium efflux from neurons, phenytoin sodium tends to stabilise the threshold against hyperexcitability caused by environmental changes or excessive stimulation capable of reducing membrane sodium gradient. This includes the reduction of post tetanic potentiation of synapses. Loss of post tetanic potentiation prevents cortical seizure foci from detonating adjacent cortical areas. Phenytoin thereby reduces the over-activity of brain stem centres responsible for the tonic phase of grand mal seizures. Phenytoin sodium’s antiarrhythmic action may be attributed to the normalization of influx of sodium and calcium to cardiac Purkinje fibres. Abnormal ventricular automaticity and membrane responsiveness are decreased. It also shortens the refractory period, and therefore shortens the QT interval and the duration of the action potential. Hydantoins induce production of liver microsomal enzymes, thereby accelerating the metabolism of concomitantly administered drugs.
PHARMACOKINETICS :
Phenytoin is slowly but almost completely absorbed from the gastrointestinal tract. It is largely insoluble at the acid pH of the stomach, most being absorbed from the upper intestine; the rate of absorption is variable and is reported to be affected by the presence of food. Absorption after intramuscular injection is slower than that from the gastrointestinal tract. Phenytoin is extensively metabolised in the liver to inactive metabolites, chiefly 5-(4 hydroxyphenyl)-5-phenylhydantoin. The rate of metabolism appears to be subject to genetic polymorphism and may also be influenced by racial characteristics; it is reported to be increased during pregnancy and menstruation and to decrease with age. Phenytoin hydroxylation is saturable and is therefore readily inhibited by drugs that compete for its metabolic pathways; this is also the reason why small increments in dose may produce large rises in plasma concentration. Phenytoin undergoes enterohepatic recycling and is excreted in the urine, mainly as its hydroxylated metabolite, in either free or conjugated form.
Phenytoin is widely distributed throughout the body. It is about 90 % bound to plasma proteins, although this may be reduced in certain disease states and in certain patient populations (see Precautions, below). It has a very variable, dose-dependent half-life, but the mean plasma half-life appears to be about 22 hours at steady state; because phenytoin inhibits its own metabolism it may sometimes be several weeks before a steady-state plasma-Phenytoin concentration is attained. Monitoring of plasma concentrations may be performed as an aid in assessing control, and the therapeutic range of total plasma Phenytoin concentrations is usually quoted as 10 to 20 micrograms/ml (40 to 80 micromoles/litre); some patients, however, achieve control at concentrations outside this range. It has been suggested that, because of differences in protein binding, measurement of free phenytoin concentrations in plasma may prove more reliable; measurement of concentrations in saliva, which contains only free phenytoin, has also been performed. Phenytoin crosses the placental barrier and small amounts are distributed into breast milk. The pharmacokinetics of phenytoin are affected by other antiepileptics (see Precautions, below).
INDICATIONS :
Epilepsy :
Control of tonic-clonic (grand mal) seizures and partial seizures (focal including temporal lobe) or a combination of these. Treatment of seizures occurring during or following neurosurgery and/or severe head injury. Treatment of trigeminal neuralgia but only as a second line therapy if carbamazepine is ineffective or patients are intolerant of carbamazepine.
Administration :
For oral use.
Dosage :
Recommended Dosage :
92 mg of phenytoin is equivalent to 100 mg of Phenytoin sodium. Dosage should be individually titrated as there may be wide variability in phenytoin serum levels with equivalent dosage. Phenytoin should be introduced in small doses with gradual increments until control is achieved or until toxic effects appear. The clinically effective plasma phenytoin concentration is 10-20 μg/ml (40-80 μmol/litre) but some patients are satisfactorily controlled at concentrations outside this range.
Adults :
Initially 3 to 4 mg/kg/day with subsequent dosage adjustment as necessary. The usual maintenance dose is 200 to 500 mg daily in single or divided doses.
Children and Infants :
Initially 5 mg/kg/day in 2 or 3 divided doses. A suggested maintenance dose is 4 to 8 mg/kg daily in divided doses. Maximum dosage is 300 mg daily.
Neonates :
In neonates the absorption of phenytoin following oral administration is variable and the metabolism of phenytoin may be depressed. It is therefore very important to monitor serum levels in the neonate.
Administration in liver disorders :
A reduced dose should be used to avoid toxicity.
Elderly :
The usual adult dose unless serum albumin is low or hepatic or renal dysfunction is present. If it is necessary to transfer a patient from phenytoin to other anticonvulsant therapy, this is best effected over a period of one week with gradual withdrawal of phenytoin.
CONTRAINDICATIONS :
Hypersensitivity to Phenytoin, other hydantoins, or any of the excipients.
Suicidal ideation and behaviour have been reported in patients treated with anti-epileptic agents in several indications. A meta-analysis of randomised placebo controlled trials of anti-epileptic drugs has also shown a small increased risk of suicidal ideation and
behaviour. The mechanism of this risk is not known and the available data do not exclude the possibility of an increased risk for phenytoin sodium. Therefore patients should be monitored for sings of suicidal ideation and behaviours and appropriate treatment should be considered. Patients (and caregivers of patients) should be advised to seek medical advice should signs of suicidal ideation or behaviour emerge. Care should be taken in treating patients with phenytoin if they have alcoholism, diabetes mellitus, blood dyscrasias, hepatic, renal or thyroid function impairment or febrile illness with a temperature above 38°C for more than 24 hours. Patients or their carers should be told how to recognize signs of blood or skin disorders, and are advised to seek immediate medical attention if symptoms such as fever, sore throat, rash, mouth ulcers, bruising or bleeding develop. If a rash occurs treatment should be discontinued: if the rash is mild re-introduce cautiously but discontinue immediately if recurrence. Leukopenia, which is severe, progressive or associated with clinical symptoms, requires withdrawal (if necessary under cover of a suitable alternative).
Phenytoin is highly protein bound and extensively metabolised by the liver. Reduced dosage to prevent accumulation and toxicity may therefore be required in patients with impaired liver function. Protein binding may be reduced in certain disease states such as uraemia, and in certain patient populations such as neonates and the elderly. The resulting elevation of free phenytoin may not necessarily require a change in dosage of phenytoin although relatively lower total plasma phenytoin concentrations will be found to be effective since there is less bound phenytoin available for measurement. Patients with impaired liver function, the elderly or gravely ill may show early signs of toxicity. Patients with renal abnormalities or hypoalbuminaemia associated with AIDS may have an increased risk of elevated free phenytoin concentrations and subsequent toxicity. Phenytoin is not effective for absence (petit mal) seizures. If tonic-clonic (grand mal) and absence seizures are present together, combined drug therapy is needed. Phenytoin may affect glucose metabolism and inhibit insulin release. Hyperglycaemia has been reported in association with toxic levels. Phenytoin is not indicated for seizures due to hypoglycaemia or other metabolic causes. Plasma levels of Phenytoin sustained above the optimal range may produce confusional states. At the first sign of acute toxicity, plasma drug level determinations are recommended. Dose reduction of phenytoin therapy is indicated if plasma levels are excessive; if symptoms persist, termination of therapy with phenytoin is recommended.
Phenytoin therapy may interfere with Vitamin D metabolism (Refer Interactions). In the absence of an adequate dietary intake of Vitamin D or exposure to sunlight, osteomalacia, hypocalcaemia or rickets may develop. Phenytoin induces the CYP450 enzyme which affects bone metabolism indirectly by increasing metabolism of vitamin D3. Increased metabolism of vitamin D3, induced by phenytoin, may lead to vitamin D deficiency and heightened risk of osteomalacia, bone fractures, osteoporosis and hypophosphataemia in chronically treated epileptic patients. Phenytoin should be used with caution in patients with porphyria as it may exacerbate the disease. (Refer Contraindications regarding acute intermittent porphyria). Patients should be monitored whilst being treated with phenytoin. Complete blood cell and platelet counts and serum biochemistry including liver function tests should be performed periodically. Dental examinations are recommended at regular intervals for teeth cleaning and reinforcement of patient’s plaque control for inhibition of gingivial hyperplasia. EEGs, serum phenytoin and folate levels and physical examination paying special attention to the lymph glands and skin should also be undertaken periodically. Thyroid function determinations are recommended during the first few months of treatment to detect symptoms of hypothyroidism which may be unmasked by phenytoin.
Dosage reduction, discontinuation or substitution of an alternative antiepileptic should be done gradually. Gradual withdrawal is recommended as abrupt discontinuation in a responsive epileptic patient may result in convulsions and possibly status epilepticus. If treatment with phenytoin has to be withdrawn abruptly, the changeover to another anticonvulsant agent should, if necessary, be effected under the cover of benzodiazepines. In the event of an allergic or hypersensitivity reaction, rapid substitution of alternative therapy may be necessary. In this case, alternative therapy should be an anti-epileptic drug not belonging to the hydantoin chemical class. Life-threatening cutaneous reactions Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) have been reported with the use of phenytoin. Patients should be advised of the signs and symptoms and monitored closely for skin reactions. The highest risk for occurrence of SJS or TEN is within the first weeks of treatment. If symptoms or signs of SJS or TEN (e.g. progressive skin rash often with blisters or mucosal lesions) are present, phenytoin treatment should be discontinued. Patients should be alert for signs and symptoms of hypersensitivity such as itching; and should seek immediate medical advice on observing them. The best results in managing SJS and TEN come from early diagnosis and immediate discontinuation of any suspect drug. Early withdrawal is associated with a better prognosis. If the patient has developed SJS or TEN with the use of phenytoin, Phenytoin must not be re-started in this patient at any time. If a rash is of the milder type (measles-like or scarlatiniform), Phenytoin therapy may be resumed after the rash has completely disappeared. If the rash recurs further Phenytoin medication is contraindicated. Black patients may be at increased risk of hypersensitivity reactions (including skin rash, SJS, TEN and hepatotoxicity).
Antiepileptic Hypersensitivity Syndrome (AHS) :
Antiepileptic Hypersensitivity Syndrome (AHS) is a rare drug induced, multiorgan syndrome which is potentially fatal and occurs in some patients taking anticonvulsant medication. It is characterized by fever, rash, lymphadenopathy, and other multiorgan pathologies, often hepatic. The mechanism is unknown. The interval between first drug exposure and symptoms is usually 2-4 weeks but has been reported in individuals receiving anticonvulsants for 3 or more months. Patients at higher risk for developing AHS include black patients,
patients who have a family history of or who have experienced this syndrome in the past, and immuno-suppressed patients. The syndrome is more severe in previously sensitized individuals in whom the reaction may occur within one day of re-challenge. If a patient is diagnosed with AHS, discontinue the Phenytoin and provide appropriate supportive measures. Patients with rare hereditary problems of fructose intolerance, glucose-galactose malabsorption or sucrase-isomaltase insufficiency should not take this medicine.
Pregnancy :
Specialist advice should be given to women who are of childbearing potential. If pregnancy is planned, the risks of phenytoin must be compared to the risk of discontinuing treatment. Phenytoin crosses the placenta. In view of the increased risk of neural tube defects and other congenital malformations associated with phenytoin, women taking antiepileptic drugs who intend to become pregnant or become pregnant should be counselled and offered antenatal screening. To counteract the risk of neural tube defects, adequate folate supplements are advised for women before and during the first trimester. Other reported congenital abnormalities include the fetal hydantoin syndrome symptoms of which include intrauterine growth retardation, microcephaly, underdeveloped nails on fingers and toes, developmental delay and craniofacial abnormalities). Congenital heart defects, urogenital defects, cleft lip and/or palate have also been reported. The features of foetal hydantoin syndrome are all interrelated and are frequently associated with intrauterine growth retardation from other causes. Phenytoin should only be used during pregnancy, especially early pregnancy, if in the judgement of the physician the potential benefits clearly outweigh the risk.
The frequency of seizures may increase during pregnancy in some women. This may be due to altered phenytoin absorption or metabolism. During pregnancy, caution is needed in interpreting plasma concentrations as total plasma concentrations of Phenytoin may fall, particularly in the later stages, but free plasma concentrations may remain the same or even rise. Periodic measurement of serum phenytoin levels is valuable in the management of a pregnant epileptic patient as a guide to adjustment of dose. However, postpartum restoration of the original dose will probably be indicated. Genetic factors or the epileptic condition itself may be more important than drug therapy in leading to birth defects. It is important to note that anticonvulsant drugs should not be discontinued in patients in whom the drug is administered to prevent major seizures because of the strong possibility of precipitating status epilepticus with attendant hypoxia and threat to life. In individual cases where the severity and frequency of the seizure disorders are such that the removal of medication does not pose a serious threat to the patient, discontinuation of the drug may be considered prior to and during pregnancy although it cannot be said with any confidence that even minor seizures do not pose some hazard to the developing embryo or foetus.
Exposure to phenytoin prior to delivery may lead to an increased risk of haemorrhage in the neonate, usually within 24 hours of the birth. Phenytoin may also produce a deficiency of vitamin K in the mother causing increased maternal bleeding during delivery. Risk of maternal and infant bleeding may be reduced by administration of vitamin K prophylactically to the mother one month prior to and during delivery and to the neonate intravenously immediately after birth. Neuroblastoma as well as other neuroectodermal and non-ectodermal tumours have been seen in neonates and children exposed to phenytoin prenatally. It is possible that there is an increased risk of neuroblastoma in children with fetal hydantoin syndrome.
Nursing mothers :
Phenytoin is excreted in breast milk. Infant breast-feeding is not recommended. The benefits of breast-feeding should be weighed against the possibility of an adverse effect occurring in the infant.
INTERACTIONS :
Alcohol :
Acute alcohol intake may increase phenytoin serum levels while chronic alcoholism may decrease serum levels.
Alcohol or Opioid Dependence Drugs :
Concomitant administration of phenytoin with disulfiram may result in increased plasma phenytoin levels. Also chronic phenytoin medication may increase methadone metabolism and may precipitate withdrawal symptoms in patients being treated for opioid dependence.
Anaesthetics :
Chronic use of phenytoin prior to anaesthesia may increase the metabolism of the anaesthetics enflurane, halothane and methoxyflurane.
Analgesics :
Aspirin, phenylbutazone and possibly other NSAIDS increase plasma Phenytoin concentrations. The metabolism of paracetamol may be increased in patients taking Phenytoin which may reduce the therapeutic effect of paracetamol. Isolated reports of unexpected paracetamol hepatotoxicity have been described in patients taking phenytoin.The concomitant use of azapropazone should be avoided.
Antacids :
May reduce phenytoin absorption, phenytoin plasma levels, and seizure control. Concurrent use need not be avoided but separation of the dosages by two to three hours may minimise such effects. Concurrent use of Phenytoin with any dosage forms containing calcium may decrease the bioavailability of both and should be taken one to three hours apart.
Anthelmintics :
Phenytoin may reduce plasma mebendazole concentration and significantly reduce plasma praziquantel concentration.
Antiarrhythmics :
The therapeutic effect of disopyramide, mexiletine and quinidine is decreased by concurrent phenytoin administration. Concomitant administration of amiodarone may result in increased plasma Phenytoin levels.
Side effects are fairly frequent in patients receiving phenytoin but some disappear with dose reduction or continued administration.
Blood and lymphatic system disorders :
Fatal haematopoietic complications have occasionally been reported in association with Phenytoin administration. Haematological reactions include eosinophilia, thrombocytopenia, leucopenia, granulocytopenia, agranulocytosis, pancytopenia with or without bone marrow suppression and aplastic anaemia. Macrocytosis and megaloblastic anaemia have occurred but these conditions usually respond to folate therapy. A relationship has been suggested between phenytoin treatment and development of lymphadenopathy including benign lymph node enlargement, pseudolymphoma, lymphoma and Hodgkin’s disease. The occurrence of lymphadenopathy (local and generalised) indicates the need to differentiate such a condition from other types of lymph node pathology. Lymph node involvement may occur with or without symptoms and signs resembling serum sickness, e.g. fever, rash and liver involvement. In all cases of lymphadenopathy, follow-up observation for an extended period is indicated and every effort should be made to achieve seizure control using alternative antiepileptic drugs.
Immune system disorders :
Anaphylactoid reactions and anaphylaxis.
Antiepileptic Hypersensitivity Syndrome (AHS) :
A rare drug induced, multiorgan syndrome which is potentially fatal, comprising serum sickness (fever, rash, lymphadenopathy, arthralgia and urticaria) and less commonly lymphocytosis, and liver and other organ involvement such as renal failure, has been associated with some antiepileptic drugs including phenytoin. Clinical manifestations include interstitial nephritis, anaemia, interstitial pulmonary infiltrates, pneumonitis, thrombocytopenia, eosinophilia, myopathy, polyarteritis nodosa and diffuse intravascular coagulation. The syndrome occurs most frequently on first exposure to the drug, with initial symptoms starting anywhere between 1 and 8 weeks after exposure (Refer Warnings and Precautions). Hypersensitivity reactions include hepatic necrosis. Possible increased incidence of hypersensitivity reactions (including skin rash and hepatotoxicity) in black patients.
Nervous system disorders :
Common side effects include headache, dizziness, transient nervousness, and insomnia. The most common undesirable effects encountered with phenytoin are related to the central nervous system as a syndrome of cerebellar, vestibular and ocular effects, notably nystagmus, diplopia and ataxia, and may be asscociated with exacerbation of seizure frequency and reversible hyperglycaemia. CNS side effects are usually dose related and also slurred speech, mental confusion, motor twitching, paraesthesia, somnolence and drowsiness. There are also rare reports of phenytoin induced dyskinesias including chorea, dystonia, tremor and asterixis. Occasionally irreversible cerebellar dysfunction and peripheral neuropathy have been reported. Prolonged therapy may produce subtle effects on mental function and cognition, especially in children. A predominantly sensory polyneuropathy has been observed in patients receiving long-term Phenytoin therapy.
Gastrointestinal disorders :
Common side effects include lack of appetite, nausea, vomiting or constipation. Tenderness and hyperplasia of the gums often occurs, particularly in younger patients. Rarely, salivary gland enlargement.
Hepatobiliary disorders :
Hepatitis, liver damage.
Skin and subcutaneous tissue disorders :
Dermatological side effects are sometimes accompanied by fever and include acne, scarlatiniform or morbilliform rashes. Bullous, exfoliative or purpuric dermatitis, lupus eyrthematosus, and erythema multiforme are rare events. Severe cutaneous adverse reactions (SCARs) : Stevens-Johnson syndrome and toxic epidermal necrolysis have been reported very rarely.
Musculoskeletal and connective tissue disorders :
Polyarthropathy. There have been reports of decreased bone mineral density, osteopenia, osteoporosis and fractures in patients on long-term therapy with phenytoin. The mechanism by which phenytoin affects bone metabolism has not been identified. Connective tissue side effects include coarsening of the facial features, enlargement of lips Peyronie’s disease and Dupuytren’s contracture.
Reproductive system and breast disorders :
Gynaecomastia. Hirsutism.
Investigations :
Plasma calcium may be lowered which can lead to rickets or osteomalacia. Phenytoin can also cause significant reduction in 25-hydroxycholecalciferol concentrations and elevated alkaline phosphatase. phenytoin may increase high-density lipoprotein (HDL) cholesterol and plasma triglyceride concentrations.
EFFECTS ON ABILITY TO DRIVE AND USE MACHINES :
Phenytoin causes dizziness and drowsiness. Patients should not drive or operate machinery if affected. Driving by patients with epilepsy is legally regulated and restricted to those whose seizures are adequately controlled.
OVERDOSAGE :
Symptoms :
The lethal dose in children is not known. The mean lethal dose in adults is estimated to be 2 to 5 g. Initial symptoms and signs of overdose include blurred vision, nystagmus, ataxia, dysarthria and seizures. Coma, fixed dilatation of pupils hypotension and apnoea then follow. Death is due to respiratory and circulatory depression. Reports of irreversible cerebellar dysfunction are associated with severe overdose of phenytoin. Hyperglycaemia has also been reported with toxic levels of phenytoin. There are marked variations among individuals with respect to phenytoin serum levels where toxicity may occur. Nystagmus on lateral gaze usually appears at 20 mg/l, and ataxia at 30 mg/l, dysarthria and lethargy appear when the serum concentration is greater than 40 mg/l, but a concentration as high as 50 mg/l has been reported without evidence of toxicity.
TREATMENT OF OVERDOSAGE :
There is no specific antidote. Maintain a clear airway and ensure adequate ventilation. The benefit of gastric decontamination is uncertain. Consider activated charcoal if the patient presents within 1 hour of ingestion of 20 mg/kg or more phenytoin, provided the airway can be protected. Consider repeated doses of oral activated charcoal, provided the patient is not vomiting and the airway can be protected. Treatment should then be supportive and symptomatic, fluid, cardiorespiratory, hepatic, renal and blood glucose statuses should be monitored. Oxygen and assisted ventilation may be necessary for central nervous system (CNS), respiratory and cardiovascular depression. Haemodialysis and haemoperfusion are of doubtful clinical efficacy. Peritoneal dialysis is not effective. Total exchange transfusion has been utilised in the treatment of severe intoxication in children. In acute overdosage the possibility of the presence of other CNS depressants, including alcohol, should be bourne in mind.
STORAGE :
Stored below 30°C (86°F), protected from moisture and light. Do not refrigerate. PHENYTOIN SODIUM is slightly hygroscopic means it ready picks up and retains moisure. Do not store these tablets in bathroom or kitchen where there is higher incidence of moisture in the air. Note : Do not remove dessicants (small canisters containing drying agent) from the pack. Dessicants are provided to protect the drug from moisture and they are not to be consumed.
SHELF LIFE :
24 months from the date of manufacture.
PRESENTATION :
PHENYTOIN TABLETS B.P. contains Phenytoin Sodium B.P.
100 mg.
250 Tablets are packed in a Bottle.
Disclaimer : For the use of a Registered Medical Practitioner or a Hospital or a Institution only. Also it is not intended to be used by healthcare professionals or patients for the purpose of prescribing or administering these products. Questions regarding the complete and current content of product labeling / specification / presentation should be directed to SGPharma.

 Cardiovascular
Cardiovascular





