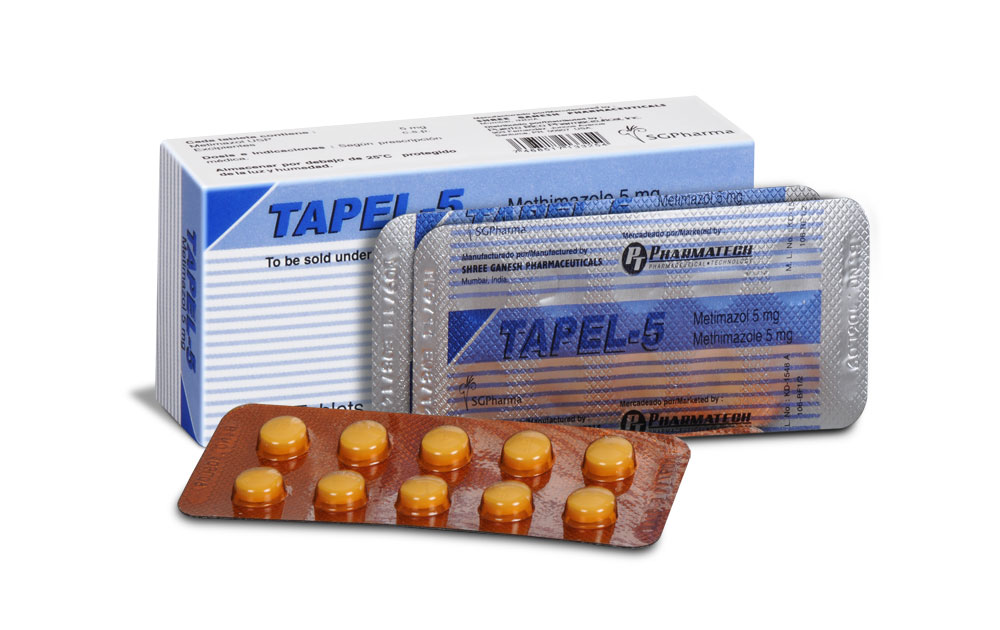
5 mg, 10 mg, 20 mg
For the use of a Registered Medical Practitioner or a Hospital or a Institution only.
TAPEL (Methimazole) is an orally administered thiourea antithyroid drug. Chemically, Methimazole is 1-methylimidazole-2-thiol. It differs chemically from the drugs of the thiouracil series primarily because it has a 5-membered ring instead of a 6. The molecular formula is C4H6N2S and the molecular weight is 114.16.
STRUCTURAL FORMULA :
Its structural formula is :
-STRUCTURE.jpg)
TAPEL - 5 mg tablets are white in colour, round, beveled, scored and debosed with SGP on one side.
TAPEL - 10 mg tablets are white in colour, round, beveled, scored and debosed with SGP on one side.
TAPEL - 20 mg tablets are white in colour, round, beveled, scored and debosed with SGP on one side.
COMPOSITION :
Tapel-5
Each tablet contains :
Methimazole USP 5 mg
Excipients q.s.
Tapel-10
Each tablet contains :
Methimazole USP 10 mg
Excipients q.s.
TAPEL-20
Each tablet contains :
Methimazole USP 20 mg
Excipients q.s.
ACTIONS :
Methimazole inhibits the synthesis of thyroid hormones and thus is effective in the treatment of hyperthyroidism. The drug dose not inactivate existing thyroxine and triiodothyronine that are stored in the thyroid or circulating in the blood nor does it interfere with the effectiveness of thyroid hormones given by mouth or by injection. The actions and use of Methimazole are similar to those of propylthiouracil. On a weight basis, the drug is at least 10 times as potent as propylthiouracil, but Methimazole may be less consistent in action.
PHARMACOKINETICS :
Methimazole is readily absorbed from the gastrointestinal tract. It is metabolized rapidly and requires frequent administration. Methimazole is not bound to plasma proteins. Methimazole has an eliminiation half life from plasma of about 3 to 6 hours & is metabolised, probably by the liver & excreted in the urine. Less than 12 % of a dose of Methimazole may be excreted as unchanged drug. 3-methyl-2-thiohydantoin has been identified as a metabolite of Methimazole. The elimination half-life may be increased in hepatic & renal impairment.
INDICATIONS :
TAPEL is indicated in the medical treatment of hyperthyroidism, including the treatment of Graves disease, long-term therapy may lead to remission of the disease. TAPEL may be used to ameliorate hyperthyroidism in preparation for subtotal thyroidectomy or radioactive iodine therapy. TAPEL is also used when thyroidectomy is contraindicated or not advisable.
TAPEL is administered orally. Tablets are usually given in three equal doses at approximately 8-hour intervals.
Adult :
The initial daily dosage is 15 mg for mild hyperthyroidism, 30 to 40 mg for moderately severe hyperthyroidism and 60 mg for severe hyperthyroidism, divided into 3 doses at 8-hour intervals. The maintenance dosage is 5 to 15 mg daily.
Paediatric :
Initially, the daily dosage is 0.4 mg/kg of body weight divided into 3 doses and given at 8-hour intervals. The maintenance dosage is approximately half of the initial dose.
CONTRAINDICATIONS :
TAPEL is contraindicated in the presence of hypersensitivity to the drug and in nursing mothers because the drug is excreted in milk.
WARNINGS :
Agranulocytosis is potentially a serious side effect. Patients should be instructed to report to their physicians any symptoms of agranulocytosis, such as fever or sore throat. Leukopaenia, thrombocytopaenia and aplastic anaemia (pancytopaenia) may also occur. The drug
should be discontinued in the presence of agranulocytosis, aplastic anaemia (pancytopaenia), hepatitis or exfoliative dermatitis. The patients bone marrow function should be monitored. Due to the similar hepatic toxicity profiles of TAPEL and propylthiouracil, attention is drawn to the severe hepatic reactions which have occurred with both drugs. There have been rare reports of fulminant hepatitis, hepatic necrosis, encephalopathy and death. Symptoms suggestive of hepatic dysfunction (anorexia, pruritus, right upper quadrant pain, etc) should prompt evaluation of liver function. Drug treatment should be discontinued promptly in the event of clinically significant evidence of liver abnormality including hepatic transaminase values exceeding 3 times the upper limit of normal.
Pregnancy : Category D
TAPEL can cause foetal harm when administered to a pregnant woman. TAPEL readily crosses the placental membranes and can induce goiter and even cretinism in the developing foetus. In addition, rare instances of congenital defects : aplasia cutis, as manifested by scalp defects; oesophageal atresia with tracheoesophageal fistula and choanal atresia with absent/hypoplastic nipples, have occurred in infants born to mothers who received TAPEL during pregnancy. If TAPEL is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be warned of the potential hazard to the foetus. Since the above congenital defects have been reported in offspring of patients treated with TAPEL, it may be appropriate to use other agents in pregnant women requiring treatment for hyperthyroidism.The drug appears in human breast milk and its use is contraindicated in nursing mother. Postpartum patients receiving TAPEL should not nurse their babies.
PRECAUTIONS :
General :
Patients who receive TAPEL should be under close surveillance and should be cautioned to report immediately any evidence of illness, particularly sore throat, skin eruptions, fever, headache, or general malaise. In such cases, white-blood-cell and differential counts should be made to determine whether agranulocytosis has developed. Particular care should be exercised with patients who are receiving additional drugs known to cause agranulocytosis.
Laboratory Tests :
Because TAPEL may cause hypoprothrombinaemia and bleeding, prothrombin time should be monitored during therapy with the drug, especially before surgical procedures. Periodic monitoring of thyroid function is warranted and the finding of an elevated TSH warrants a decrease in the dosage of TAPEL.
INTERACTIONS AND INCOMPATIBILITIES :
Anticoagulants (oral) :
The activity of oral anticoagulants may be potentiated by anti-vitamin-K activity attributed to Methimazole.
ß-adrenergic blocking agents :
Hyperthyroidism may cause an increased clearance of beta ratio. A dose reduction of beta-adrenergic blockers may be needed when a hyperthyroid patient becomes euthyroid.
Digitalis glycosides :
Serum digitalis levels may be increased when hyperthyroid patients on a stable digitalis glycosides regimen become euthyroid; reduced dosage of digitails glycosides may be required.
Theophylline :
Theophylline clearance may decrease when hyperthyroid patients on a stable theophylline regimen become euthyroid; a reduced dose of theophylline may be needed.
SIDE EFFECTS :
Major adverse reactions (which occur with much less frequency than the minor adverse reactions) include inhibition of myelopoieses (agranulocytosis, granulocytopaenia and thrombocytopaenia), aplastic anaemia, drug fever, a lupuslike syndrome, insulin autoimmune syndrome (which can result in hypoglycaemic coma), hepatitis (jaundice may persist for several weeks after discontinuation of the drug), periarteritis and hypoprothrombinaemia. Nephritis occurs very rarely. Minor adverse reactions include skin rash, urticaria, nausea, vomiting, epigastric distress, arthralgia, paresthesia, loss of taste, abnormal loss of hair, myalgia, headache, pruritus, drowsiness, neuritis, oedema, vertigo, skin pigmentation, jaundice, sialadenopathy and lymphadenopathy. It should be noted that about 10 % of patients with untreated hyperthyroidism have leukopaenia (white-blood-cell count of less than 4,000/mm3), often with relative granulopaenia
OVERDOSAGE :
Symptoms of overdosage may include nausea, vomiting, epigastric distress, headache, fever, joint pain, pruritus and oedema. Aplastic anaemia (pancytopaenia) or agranulocytosis may be manifested in hours to days. Less frequent events are hepatitis, nephrotic syndrome, exfoliative dermatitis, neuropathies and CNS stimulation or depression. Although not well studied, Methimazole-induced agranulocytosis is generally associated with doses of 40 mg or more in patients older than 40 years of age.
TREATMENT OF OVERDOSAGE :
In managing overdosage, consider the possibility of multiple drug overdoses interaction among drugs, and unusual drug kinetics in your patient. Protect the patients airway and support ventilation and perfusion. Meticulously monitor and maintain, within acceptable limits, the patients vital signs, blood gases, serum electrolytes, etc. The patients bone marrow function should be monitored. Absorption of drugs from the gastrointestinal tract may be decreased by giving activated charcoal, which, in many cases, is more effective than emesis or lavage ; consider charcoal instead of or in addition to gastric emptying. Repeated doses of charcoal over time may hasten elimination of some drugs that have been absorbed. Safeguard the patients airway when employing gastric emptying or charcoal. Forced diuresis, peritoneal dialysis, haemodialysis or charcoal haemoperfusion have not been established as beneficial for an overdose of Methimazole.
STORAGE :
Store below 30°C (86°F), protected from moisture and light.
SHELF LIFE :
24 months from date of manufacture.
PRESENTATION :
TAPEL tablets contain Methimazole USP
5 mg /10 mg /20 mg.
3 blisters of 10 tablets per box.
Disclaimer : For the use of a Registered Medical Practitioner or a Hospital or a Institution only. Also it is not intended to be used by healthcare professionals or patients for the purpose of prescribing or administering these products. Questions regarding the complete and current content of product labeling / specification / presentation should be directed to SGPharma.

 Cardiovascular
Cardiovascular